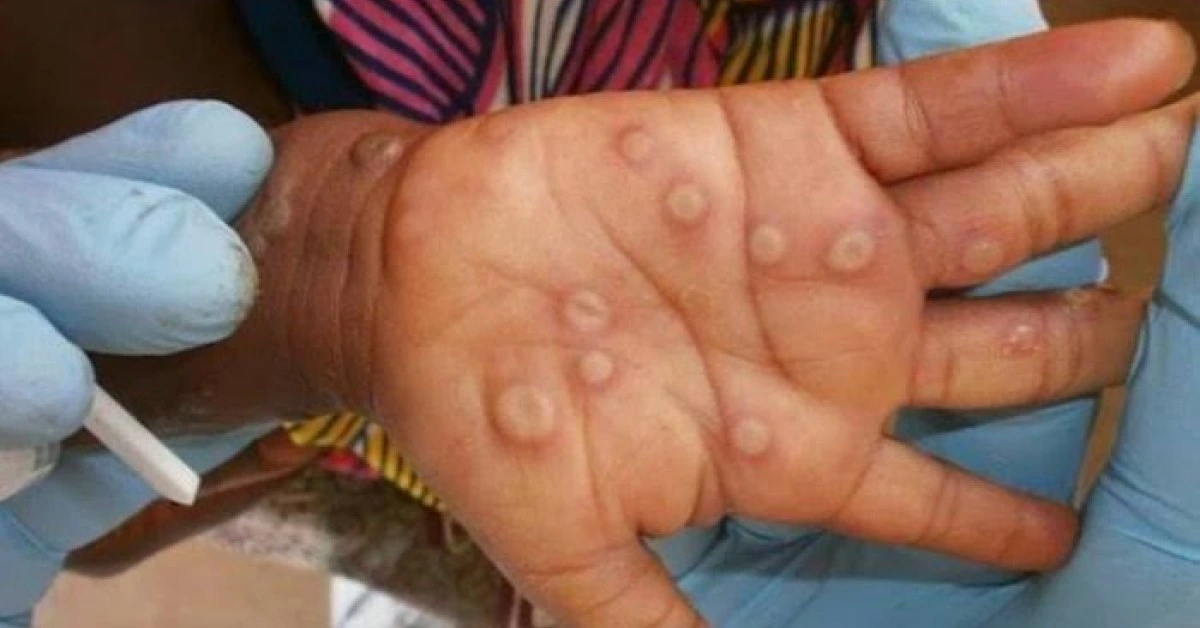
DRC – A new and potentially more infectious variant of mpox, Clade 1A, has been identified in the Democratic Republic of the Congo (DRC), according to Dr. Ngashi Ngongo, head of the mpox incident management team at the Africa Centre for Disease Control and Prevention (Africa CDC).
However, efforts to test and monitor the disease are being severely impacted by violence in eastern DRC and the recent termination of U.S. foreign aid. With only 35% of mpox cases currently being tested, the true scale of the outbreak remains uncertain.
This week, the DRC launched its first vaccination campaign in Kinshasa, with a rapid response that saw over 24,800 people vaccinated in just four days.
Despite these efforts, mpox continues to spread in Uganda, which has seen a steady rise in cases for three consecutive weeks, with 278 new cases reported in the past week alone.
Overcrowded health facilities are struggling to manage patients, with a treatment center in Entebbe, designed for 80 patients, currently housing 102. To cope, the Ugandan Ministry of Health has introduced home-based care for mild cases.
In South Africa, which had been mpox-free for over 90 days, three new cases have emerged. The World Health Organization (WHO) has decided to maintain mpox as a public health emergency of international concern, citing rising case numbers, geographic spread, insecurity in eastern DRC, and lack of funding for response efforts.
Meanwhile, Kenya continues to battle an mpox outbreak that was first declared on July 31, 2024. As of February 21, 2025, the country has recorded 48 confirmed cases and one death.
The outbreak has spread across 12 counties, with notable transmission along the A104 trade corridor, primarily affecting truck drivers and sex workers.
The presence of the more severe Clade 1B strain raises concerns about further spread within East Africa.
Although Kenya has activated an Incident Management System (IMS), strengthened screening, and mobilized resources, authorities emphasize the need for improved cross-border coordination and targeted vaccination strategies.
Dr. Jean Kaseya, Director-General of Africa CDC, has warned of the escalating crisis, stating, “We are playing with fire.”
He emphasized that while much of the world has moved past the 2022–2023 global mpox outbreak, Africa remains heavily affected, with the DRC serving as the epicenter.
The country has been reporting over 2,000 suspected cases weekly for months. Although case numbers appeared to drop in late January, experts believe this decline reflects disruptions in monitoring and reporting rather than a real decrease in infections.
Ongoing conflict in eastern DRC, where rebel forces have seized control of key areas, has significantly hindered response efforts.
Additionally, the recent freeze in U.S. foreign aid—following the decision by the Trump administration to cut off USAID funding and withdraw from the WHO—has stalled critical aspects of the mpox response, leaving African nations struggling to control the outbreak.
A former U.S. response team health worker, speaking anonymously, described the situation as “watching a train wreck in real time—and not being able to do a thing about it.”
New febrile disease outbreak in DRC
Alongside the mpox crisis, health authorities in the DRC are investigating a febrile disease outbreak in five villages within the Basankusu and Bolomba health zones in Equateur province.
According to the WHO, cases have tripled in the past three weeks, with a total of 943 cases and 52 deaths reported so far.
Symptoms include fever, chills, sweating, headaches, and muscle pain. Notably, no hemorrhagic symptoms have been observed, and preliminary tests for Ebola and Marburg viruses have returned negative results.
Health experts suspect malaria as the leading cause, as rapid diagnostic tests on over 500 samples showed a 55% positivity rate, while blood smear tests on 70 samples returned a nearly 78% positivity rate.
However, further investigations, including tests for meningitis and environmental contamination assessments, are ongoing.
Basankusu and Bolomba, located about 180 kilometers apart and over 300 kilometers from the provincial capital, Mbandaka, are difficult to access due to poor infrastructure.
Limited road networks and weak telecommunication systems further complicate health response efforts, making timely testing and treatment a challenge.
XRP HEALTHCARE L.L.C | License Number: 2312867.01 | Dubai | © Copyright 2025 | All Rights Reserved